
An ultrasound-guided ulnar nerve block can be performed to give surgical anesthesia or analgesia to the ulnar side of the hand and the little finger and the ring finger. It is most helpful in ulnar nerve distribution operations but can also use as an add-on to radial and median nerve blocks for complete hand anaesthesia, or as a supplementary to inadequately effective brachial plexus blocks. As a means of anesthesia, it is used in patients who cannot be given sedation for procedures such as fracture reductions and is also very useful in the management of acute pain in patients with burns among others. For repeated lacerations that would need suturing, regional anesthesia techniques help in reducing the total volume of local anesthetic while providing adequate surgical anesthesia to the areas.
For an ultrasound-guided ulnar nerve block, the following supplies are needed:
Local anaesthetic: 3 to 5 mL of 0. 5% bupivacaine or ropivacaine for more prolonged blockade or 3-5 ml 2 % lidocaine or 1. 5% mepivacaine for short lasting blocks.
Ultrasound scanner and high-frequency linear transducer with a frequency above 8 MHz
Sterile ultrasound gel
Bevel block needle- Short
10 mL syringe
Skin antiseptic solutions like povidone iodine solution or 2% chlorhexidine solution
Before proceeding, the clinician should seek the consent to be recorded from the patient. Ensure that the patient is positioned in a way the volar area of the affected arm is most exposed. This can be done with the forearm and hand placed on a flat surface or by bringing the arm to the right angle at the elbow while laying the forearm on the back with palms down on a stack of towels. The latter position facilitates the steadying of the arm on the towels while holding the ultrasound probe. Wash the area over the intended injection site with povidone iodine or 2% chlorhexidine. Place a sterile cover over the high frequency linear ultrasound probe and then make sure that a gel is applied to the surface of the cover. Squeeze the following local anaesthetic into a syringe of your preference. Make sure the patient is well observed, and intralipid 20% should be nearby in case the pt has systemic toxicity from the local anesthetic used.
Above or Below the Elbow Approach:
Supine Position: The patient is in a supine position and one of the patient’s arms is raised with slight abduction at the shoulder and flexion at the elbow. By fixing the forearm in pronation or supination, additional support is available and could be done by using towels or a pillow.
Seated Position: The position of the patient is sitting, and the arm is placed in slightly flexed position in order to have proper access for working on the medial aspect of the forearm.
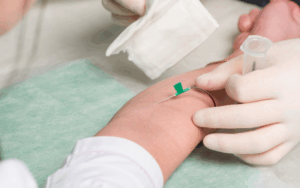
Patients forearm placed in the supine position
Step 1-Place the ultrasound probe in the horizontal plane over the medial side of the forearm slightly proximal to the medial epicondyle.
Step 2-Identify the ulnar nerve running as a white structure, resembling a honeycomb just beneath the flexor carpi ulnaris muscle.
Step 3-Identify the ulnar nerve and trace it distally ending approximately 3 to 4 cm proximal to the cubital tunnel.
Step 4-Pass the block needle in a lateral-medial fashion while always keeping the needle tip in view.
Step 5-Stab the needle tip to a position just beneath the ulnar nerve.
Step 6-It is advisable to perform negative aspiration as a way of confirming that the needle tip is not within a blood vessel if one is intended.
Step 7-Every 1-2 mL of a local anaesthetic is injected, and the position of the needle tip may be changed.
Step 8-In the case of the subcutaneous anaesthesia, repeat the process of aspiration and injection until distribution of the local anaesthesia is around the nerve is enough.
Step 9-Do not administer intraneurally: infuse the drug intravenously rather than directly into the nerve. When the needle tip appears to be in the nerve or when the patient complains of intense pain during injection, one should not proceed and should withdraw the needle.
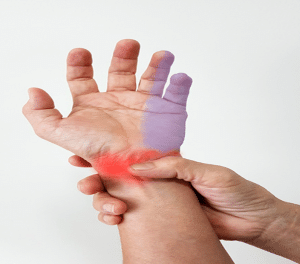
Ulnar Nerve Block
The first and most critical clinical justification for the block significantly determines the level at which the procedure should be performed. If the block occurs distal from the branching points, the nerve will remain blocked only partially or not at all. There are several sites that can be used to anesthetise the ulnar nerve: axillary, mid humeral, above or below the elbow, and wrist.
- Complete blood count
- Renal function test
- Kidney function test
- Blood glucose test
- Electrocardiogram
- Hematoma
- Infection
- Neuropathy
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



