
Subarachnoid spinal block is a safe option for general anesthesia in lower body surgeries.
This procedure temporarily blocks nerve signals to cause loss of sensation and muscle control.
The spinal cord is surrounded with three protective layers as:
The dura mater
Arachnoid mater
Pia mater
The subarachnoid space lies between the arachnoid and pia mater. It consists of cerebrospinal fluid that gives support to the spinal cord and brain.
- Spinal Needle
- Syringe
- Anesthetic Agent
- Monitoring Equipment
All necessary equipment is available in good condition including local anesthetics, syringes, and needles.
Intravenous access for fluid administration and emergency medications should be prepared. Preloading with IV fluids is done to reduce the risk of hypotension during spinal block.
Patients should follow as instructed by the physician. Fast for 6 to 8 hours before the procedure to reduce the risk of aspiration.
Informed Consent:
Patients should understand procedure, benefits, risks, and alternatives for consent.
Patient should be seated with arched back or on side for better access to lumbar spine.
The patient should be sited on the edge of the bed/table with their feet supported on a stool.
Patient positioned laterally or sitting with assistance for spinal anatomy identification, with preference for sitting due to accuracy.
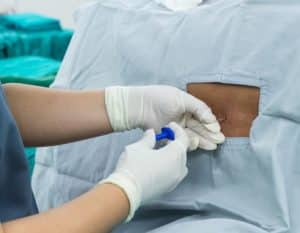
Fig. Subarachnoid spinal block
Step 1-Pre-procedure Assessment:
Check patient history including allergy history, chronic disease history, previous operation history.
Check laboratory values include platelet count and coagulation profiles.
Step 2-Preparation:
Wash the skin with an antiseptic solution.
Give the pre-procedural medicine to sedate the patient if required.
Needle Insertion: The most frequent used approach is between the L3-L4 or L4-L5 lumber vertebrae.
The needle should be inserted perpendicular to the skin, moving further through the subcutaneous tissue, ligamentum flavum, till it reaches the subarachnoid space.
Step 3-Confirmation of Needle Placement:
CSF Return: Once the needle reaches the subarachnoid space, CSF will return through the needle.
Step 4-Injection of Local Anesthetic: The anesthesiologist will slowly inject the local anesthetic, observing the patient’s response.
Step 5: Withdrawal of needle:
Withdraw the needle and cover the site with a sterile dressing.
Step 6-Patient Monitoring: Patients should be carefully observed for symptoms of increased risk of side effects such as hypotension, bradycardia, or respiratory depression.
Hypotension (Low Blood Pressure):
Due to sympathetic blockade, there is vasodilation and decreased return of blood that can lead to an abrupt drop in blood pressure.
The treatment includes fluids and vasopressors if required.
Bradycardia (Slow Heart Rate):
By spinal anesthesia, there can be an influence on the autonomic nervous system that may cause a drop-in heart rate
It can be managed with atropine or other drugs to increase the heart rate.
Respiratory Depression:
Though very rare, it can occur at high levels or with the block placed improperly impacting respiratory muscles; it happens especially when the block ascends too high.
In severe cases, mechanical ventilation is required.
Post-Dural Puncture Headache (PDPH):
This is a frequent complication, related to leakage of CSF through the site of puncture; it may cause headache worsening with sitting or standing.
Management includes hydration, caffeine, and, as needed, an epidural blood patch to seal the leak.
Infection:
Infection at the injection site or more seriously, meningitis or epidural abscess, can occur. Proper sterile techniques reduce this risk.
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



