
Polypectomy is the surgical removal of polyps which are benign growths of tissues that may arise in many locations; however, they are frequently found in the colon, stomach, uterus, or nasal passages. Polyps are mostly benign or non-cancerous growths; however certain types of polyps are seen in the colon, and these may well turn malignant if not removed at the right time. Surgical polypectomy may be diagnostic or therapeutic depending on the fact whether the polyp was removed for relief of symptoms, to prevent further development of the disease, or for histopathological examination.
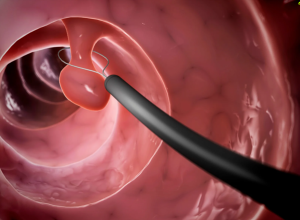
Polypectomy
Equipment
Polypectomy Snares
Cold Snares
Hot Snares
Electrosurgical Unit (ESU)
Injection Needles
Hemostatic Clips
Endoscopic Loop Devices
Baskets and Retrieval Nets
Endoscope with Channels
Patient preparation
Medical Evaluation
Medical History Review: Ask about case history of bleeding disorders, any history of allergy, present medications, and general health status. Medication Adjustments: Medications such as aspirin, warfarin, or NSAIDs that affect blood clotting might be held as a precaution against bleeding.
Pre-procedure Testing: Some patients may require microscopic analysis, for example, coagulation tests or blood tests to determine coagulation parameters and kidney function, respectively.
Dietary Restrictions
Clear Liquid Diet: More often, the day before the procedure, the patient may be required to follow a clear liquid diet.
Preoperative Management (In Preparation for Colon Polypectomy) Laxative Solution: It is then expected that a patient takes a prescribed laxative solution the morning of the procedure. This helps to empty the colon of contents making it easier to visualize the polyps.
Patient position
Left Lateral Decubitus: The patient lies on their left side with knees flexed to some extent. This position is typical of most colonoscopy cases because it allows easy bowel visibility especially if it is only the rectum and lower colon that must be examined.
Supine Position: Used sometimes if there is a desire for better visualization in different areas of the colon, for example with polyps in the ascending colon.
Bowel Preparation: The patient needs to be prepared for colonoscopy by taking a bowel wash that clears the colon. This is achieved through intermittent fasting or being on a clear liquid diet and the intake of prescription laxatives like polyethylene glycol.
Medication Review: Patients should disclose to their surgeon if they have such other medications as anticoagulant or antiplatelet because these may require alteration before the procedure.
Anesthesia: Sedation is usually given to make the patient relaxed all through the procedure.
Insertion of the Colonoscope: Endoscopy involves a colonoscope, a long, thin, flexible endoscopic tube with a focal camera and light at the tip.
The doctor carries out a visual inspection of the lining of the colon for polyps or other characteristics that may be causing bleeding.
Identification of Polyps: Polyps are classified according to their morphological appearances, that is shape, size, and color.
They can be classified into several types:
Adenomatous Polyps: These can grow into cancer. Hyperplastic Polyps: Generally benign and not associated with cancer.
Serrated Polyps: Some are benign while others can be precursors to cancer.
Snare Polypectomy: A snare (a wire loop) is used to loop around the base of the polyp.
The snare is tightened, and that tool can be used with electrocautery to remove the base of the polyp completely.
This method is applicable for bigger-sized polyps normally a size measure of greater than 1 cm.
Cold Forceps Polypectomy: Polyps of dimensions less than 5mm can be removed using a forceps method without the application of electric current.
With the help of forceps, the polyp is taken and then excised. Endoscopic Mucosal Resection (EMR):
EMR might be used for larger or more complex polyps in either technique, loops of the colon are mobilized and withdrawn through a small incision. It entails injecting a solution within the area of tissue underlying the polyp up to the time it is lifted and then snared. Endoscopic Submucosal Dissection (ESD): Larger tumor lesions, that necessitate broader invasion of tissue planes. The submucosa is then carefully separated removes the polyp en bloc.
Step 4-Specimen Collection: Polyps removed during the procedure end up being submitted to histopathological analysis to check on whether they are malignant or benign.
Step 5-Hemostasis: After polypectomy, the site is assessed for bleeding. If bleeding occurs, it can be managed with various techniques, including:
Thermal coagulation.
Hemoclips.
Argon plasma coagulation.
Step 6-Post-Procedure Care Recovery: Most patients may be observed in a specific recovery area for some time as the effect of the sedation wears off.
Post-Procedure Instructions: As for after treatment, the patients are restricted from such activities as intense movements for one or two days.
Clear liquid diets are prescribed in many cases.
Follow-Up: A routine colonoscopy may be advised depending on the number and nature of the polyps and the patient’s family history of Colorectal cancer.
Complications
Bleeding: Such can be observed during or soon after the procedure.
Delayed bleeding: This may occur up to two weeks post-procedure most specifically in the colon.
Perforation: This happens when a hole is created while operating on an organ, for instance, the colon, to remove polyps.
Risk factors: Large-sized polyps or complicated procedures or if the tissues are also weak in recovering chances are that there might be increased risks.
Infection: Though rare, infections can develop at the polyp removal site.
Post-polypectomy Syndrome
This happens when the tissue heals in a perforation-like way with symptoms of fever, pain, and tenderness but does not have a perforation.
Adverse Reactions to Anesthesia
In cases of sedation, side effects or reactions to anesthesia can occur in patients.
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



