
The thin membrane that lines the chest cavity and covers the lungs is called the pleura, and it can be removed during a pleurectomy. The pleura is made up of two layers: the parietal pleura, which lines the chest cavity, and the visceral pleura, which covers the lungs. The space between these two layers is known as the pleural cavity.
There are different types of pleurectomy procedures, and they may be performed for various reasons, including the treatment of conditions affecting the pleura. Pleurectomy may also be done as part of the treatment for certain lung diseases, infections, or tumors. The goal of pleurectomy is to remove a portion or the entirety of the pleura to address the underlying medical issue.
- Scalpel
- Scissors and Dissectors
- Forceps
- Needle Holders
- Suction Devices
- Rib Spreader
- Electrocautery or Laser Instruments
- Suture and Stapling Devices
- Chest Tubes
- Hemostatic Agents
- Anesthesia Equipment
- Informed Consent:
A comprehensive medical history is obtained, including information about existing medical conditions, previous surgeries, allergies, and medications.
- Patient Positioning:
The patient is positioned in a supine (i.e., lying on the back) position on the operating table.
Both arms may be positioned alongside the body and raised on arm boards to allow access to the chest.
Step 1: Incision
A thoracotomy incision is made, typically on the side of the chest affected by the pleural condition. The incision allows access to the pleural space.
Step 2: Rib Spreading
The ribs may be spread apart, or a rib may be removed to provide better access to the pleura.
Step 3: Pleural Exploration
The surgeon examines the pleural cavity to identify the extent of the disease, such as tumors, fibrous tissue, or effusions.
Step 4: Removal of Pleura
The surgeon then removes a portion or the entirety of the pleura, depending on the extent of the disease and the therapeutic goals.
Step 5: Closure of incision
After completing the pleurectomy, the surgeon closes the incision, and chest tubes may be inserted to drain any postoperative fluids.
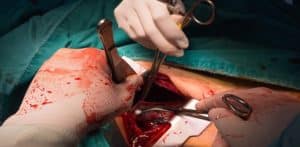
Thoracotomy incision

Closure of incision
Excessive bleeding during or after surgery can occur and may require intervention, such as reoperation or blood transfusion.
Surgical site infections or infections within the pleural space can occur. Prophylactic antibiotics are often administered before surgery to reduce the risk.
Lung infections, leading to pneumonia, may occur, particularly if there is impaired lung function or difficulty clearing secretions postoperatively.
Collapse of lung tissue may occur, especially if the patient has difficulty expanding the lungs fully after surgery. Air may accumulate in pleural space, leading to a pneumothorax. This can happen during or after surgery and may require intervention.
Postoperative respiratory complications may include difficulty breathing, decreased lung function, or the need for prolonged ventilator support.
Damage to the thoracic duct during surgery can result in the leakage of chyle into the pleural space, leading to a chylothorax. Air leakage from the lungs into the pleural space may persist after surgery, requiring additional interventions.
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



