
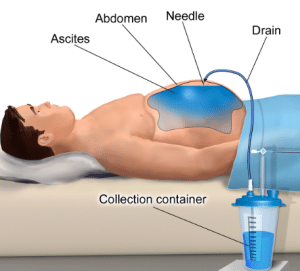
Paracentesis is a medical procedure. It removes excess fluid from the peritoneal cavity of the outer lining of the abdomen organs and abdomen. This fluid is known as ascites. Medical conditions like cirrhosis of the liver, cancer, and heart failure can lead to this. Paracentesis is performed in a clinic or hospital. A needle is inserted in the peritoneal cavity of the abdominal wall, and excess fluid is removed. Paracentesis can give relieve to discomfort and improve the breathing in individuals who have ascites. It is used to diagnose the main cause of the ascites.
The medical history of patient must be reviewed to determine if there is any factor which can increase the risk of complications from paracentesis like severe heart failure, bleeding disorders, or earlier abdominal surgery.
The current condition of patient must be checked to determine if they are stable to go for the procedure. Patient who has unstable vital sign or severe organ dysfunction may need stabilization before the procedure.
The main cause of ascites must be identified for the proper treatment plan and check for complications. This procedure is not good for patients who have chylous ascites which occurred by a leak of lymphatic fluid into peritoneal cavity.
The patients are prepared by emptying the bladder and remove any clothes which can interfere with the procedure. Ask the patient to position themself in proper and comfort pose on the examination table.
Local anesthesia is used to numb the skin at the puncture area. Sedation can be administrated to lower the discomfort and anxiety in some cases. The needle is inserted in the peritoneal cavity under the guidance of ultrasound to make sure the accurate placement of needle and to avoid any injury to internal organ.
The excessive fluid is removed to prevent complications like electrolyte imbalance or hypotension. The amount of removed fluid is dependent on the condition of patient and severity of ascites.
Monitor the patient closely after the procedure for any signs of complications like infection, bleeding, or hemodynamic instability.
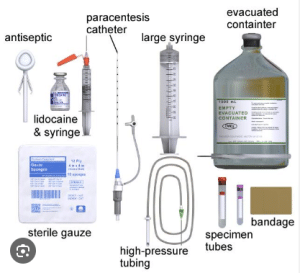
Sterile drapes and towels: These can maintain the sterile areas around the puncture site to reduce the risk of infection.
Local anesthetic: Local anesthetic like lidocaine is used to numb the skin at the puncture area to lower the discomfort and pain.
Paracentesis needle: It is a long and narrow needle with a sharp tip and side opening or trocar. It penetrates the abdominal wall and go to peritoneal cavity.
Three-way stopcock: A three-way stopcock controls the flow of fluid during the procedure. It connects the needle to the drainage bag or syringe and controls the flow rate.
Drainage tubing and bag: It connects the needle and drainage bag and collects the excess fluid from the peritoneal cavity.
Syringes: It is used to aspirate a small amount of fluid to diagnose or to administer local anesthetic.
Antiseptic solution and swabs: They are used to clean the skin at the puncture area to prevent infection.
Gauze pads and dressings: It is used to absorb any fluid which leaks from the puncture area after the procedure.
Step:1- Before the Procedure
Assessment of patients: The medical history, current condition and main cause of ascites are assessed of patients to determine if the procedure is necessary and to check for potential complications.
Informed Consent: The patient should be informed about the benefits and risks of the procedure and sign the consent form.
Pre-Procedure Preparation: The patient should empty their bladder and remove any clothes or jewelry which can interfere with the procedure. Sedation is also given to lower anxiety and discomfort.
Site Marking: The puncture area is located in the lower quadrant of abdomen which is away from blood vessels and nerves. The area is marked on the skin of the patient.
Step:2 During the Procedure
Skin Preparation: The puncture area is cleaned with an antiseptic solution to lower the risk of infection.
Local Anesthesia: Local anesthetics like lidocaine are administered into the subcutaneous tissue and skin at the puncture area to numb the skin and reduce the pain.
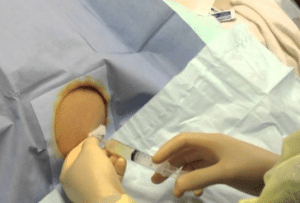
Needle Insertion: A needle is inserted in the peritoneal cavity with the help of ultrasound. This helps to see the cavity and avoid any injury to internal organs.
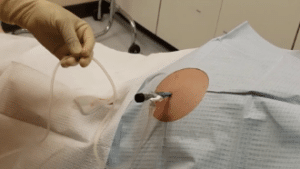
Fluid Drainage: The three-way stopcock is connected to drainage tube and needle. It is opened and excess fluid is removed slowly into the drainage tube. The flow rate is controlled as per need to prevent any complications like imbalance in electrolyte or hypotension.
Fluid Analysis: A small sample of fluid is sent to the laboratory to know the cause of ascites.
Monitoring: Monitor the patient closely after the procedure for any sign of complications like infection, bleeding, or hemodynamic instability.
Step-3: After the Procedure
Needle Removal: The needle is carefully removed, and puncture area is dressed with bandage.
Post-Procedure Care: The patient is monitored for some time after the procedure to make sure they are stable. They may need any additional fluids or medications as per need.
Follow-Up: Patient must take follow up from the healthcare provider to monitor the condition and assess further need of procedure.
Pain or discomfort at the puncture area: This is a usual side effect and stays for a few days.
Infection at the puncture site: Infection may occur if the puncture area is not properly cleaned in rare cases.
Hypotension (low blood pressure): Rapid removal of fluid may lead to hypotension which can weaken the function of heart.
Electrolyte imbalance: Sudden fluid removal may alter the levels of electrolyte which need monitoring and correction.
Hemothorax: Puncture of lung may lead to air leak into the surrounding space of lung which can lead to shortness of breathing and chest pain.
Spontaneous bacterial peritonitis (SBP): Bacteria into peritoneal cavity during the procedure may lead to SBP. It is a serious infection condition.
Severe ascites: Patients who have large amounts of ascites are at high risk of complications like imbalance in electrolyte and hypotension.
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



