
The concept of lejour technique is a procedure of breast reduction surgery that is used in the treatment of macromastia breasts. The lejour method has some advantages over the other methods for harvesting flaps; the primary goal of the lejour method is to reduce the size of the surgical incisions.
This procedure can be performed for a minor scale-down of the breast size to severe gigantomastia (mastopathy with huge breast size).
In the lejour technique, liposuction might be used to trim excess fat and breast tissue.
Scalpel
Scissors
Sutures
Liposuction cannula (if liposuction is part of the procedure)
Electrocautery (to control bleeding)
Breast tissue retractors
Implants (if breast augmentation is also being performed)
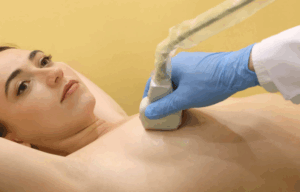
Breast examination
Consultation and physical examination: The initial step is assessment of patient medical history, and any existing prescription or over the counter medications. They will also take tests of your physical general body overview of your breasts, for instance: breast size and placements, the distance between your nipples and your sternum, and skin quality of your breasts.
Medical clearance: If you have any complications from any illness or any disease, you may require prior approval of your general practitioner prior to the surgery.
Stop smoking: Carrying excess fat can cause significant health problems, making the issue of obese weight loss a health priority for many people.
Avoid certain medications: The exclusion of some drugs before a surgery may be required; examples include aspirin and other blood thinning medicines.
Step 1: Preoperative Planning:
Consultation and Assessment: Preoperatively, the surgeon must assess the size, shape of the breast, the quality of skin, and the general health status of the candidate. In this section, patients’ course and prognosis are defined, and goals and expectations are revealed.
Marking: In marking the locations to be operated on, the patient is stood. These are the new position of the nipple and the lines made in surgery when cutting off some parts of the breasts.
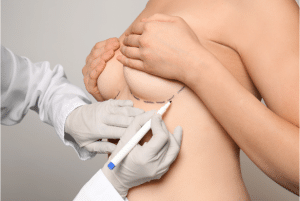
Breast marking
Step 2: Anesthesia:
General Anesthesia: The procedure is commonly done with general anesthesia since the patient may experience a lot of discomfort during the surgery.
Step 3: Incisions:
Periareolar Incision: An incision is made all the way around the areola’s perimeter.
Vertical Incision: The inframammary fold, or the crease beneath the breast, is reached via a vertical incision that descends from the areola. This is the characteristic of the short scar technique, which does not incorporate the horizontal incision along the inframammary line and surgeon’s fold, as is the case with the traditional methods.
Step 4: Tissue Removal:
Glandular and Fatty Tissue: This involves the surgery to trim out over developed or liposuction to obtain the right breast size. The totality and distribution of the tissue resection varies depending on two factors, namely the structural and morphological makeup of the patient, alongside his or her projected objectives.
Skin Resection: Surplus skin is also trimmed off to retract the resulting skin envelope and to provide the support for the new breast contour.
Step 5: Nipple-Areolar Complex (NAC) Transposition:
Nipple Repositioning: The nipple and areola tissue are elevated up and remodelled to a superior position to the patient’s younger state. In the lejour technique, the nipple and the skin cone of the areola remain connected to other tissues, such as blood vessels and nerves (pedicle).
Step 6: Reshaping and Closure:
Reshaping the Breast: The opposite breast tissue is then repositioned and moulded to achieve the desired natural look. The tissue is relocated to from a conical shape.
Suturing: Sutures are used to seal the incisions. With the vertical scar procedure, two scars are created: one vertical scar and one around the areola, forming a lollipop-shaped scar.
Step 7: Postoperative care
Dressings and Support: The breasts are vested, and sometimes an enhancing bra may be used to control expansion and enhance healing.
Follow-Up: The follow-up appointments enable the practitioner to perform check-up examinations, review recovery, and remove sutures if required, among other tasks.
Imaging tests: You may require mammograms or ultrasonograms for evaluating breasts’ health with a view to assisting the surgeon in planning the surgery.
Blood tests: Specifically, patients will undergo blood tests to allow the doctor to assess the patient’s health condition to determine they are fit for surgery.
Seroma: This is a fluid accumulation that may develop beneath the skin following surgery; it occurs when tissue swelling results from surgery, trauma, or inflammation with the buildup of extra nutrients. The management is often done by needle aspiration or drainage.
Wound healing problems: Some common adverse outcomes that may arise from operating on a patient include slow healing, development of an infection, or the wound getting worse.
Bleeding: This is commonly expected in any forms of surgery, although it is rarely significantly experienced in a breast reduction surgery.
Nipple sensation changes: Many patients who are candidates for breast reduction may experience loss or reduced sensitivity of the nipple and areola. This is often temporary, but it can be a permanent type occasionally.
Scarring: It is imperative to note that, while the lejour technique is almost perfect in terms of the reduction of scarring, the possibility of scarring still arises. This may be in form of redness and swelling at the first instance or appearing somewhat raised but will probably reduce with time.
Fat necrosis: This is a situation, which happens whereby fat cells just break down and are engulfed by the body. It can cause nodules or palpation of the breast tissues or lead to the formation of lumps in the breast.
Asymmetry: The breast can sometimes not be perfectly shaped after the process and surgery. This is one of the complications that are usual for any procedure of breast reduction mammaplasty.
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



