
Heart Transplantation is procedure of replacing failing heart with suitable donor’s heart through surgery.
Orthotopic and heterotopic heart transplants are commonly used in medical procedures. Dr. Barnard conducted first human heart transplant successfully in 1967.
Heart transplant is for patients with end-stage CHF and expected to live less than a year without it. This procedure used when other heart condition treatments unsuccessful or unavailable.
Evaluation of the heart transplant candidate includes laboratory tests and imaging studies as follows:
For laboratory tests:
Fungus and tuberculosis
Prostate-specific antigen
Papanicolaou test
Complete blood count
For imaging studies:
Coronary arteriography
Echocardiography
Posteroanterior and lateral chest radiographs
For cardiac and pulmonary evaluation:
Maximal venous oxygen consumption
Right- and left-heart catheterization
Anesthesia Equipment
Surgical Instruments
Cardiothoracic Instruments
Electrocautery Device
Donor Heart Transport Equipment
Hemostasis and Blood Management
Informed Consent:
Educate patients and their family on procedure, risks, benefits, and post-transplant regimen importance.
Recipient patient prepared for surgery with general anesthesia and baseline monitoring. Placed on cardiopulmonary bypass to assist heart and lung function during surgery.
Step 1: Removal of Donor Heart
Blood flow in the aorta is stopped with clamp, and the donor heart is cooled with cardioplegic solution during removal. Surrounding blood vessels are preserved.
Step 2: Removal of Recipient Heart
A vertical incision along the sternum gives access to the heart. Then tubes are connected to a bypass machine for pump and oxygenate blood during surgery.
Now the recipient’s heart is stopped with cardioplegic solution and that excised with back of the left atrium, pulmonary veins, right atrium, and vena cavae.
Step 3: Implantation of Donor Heart
The donor heart is carefully connected to the recipient’s major blood vessels in a specific order:
The left atrium to the recipient’s left atrial cuff, the right atrium to the right atrial cuff, the pulmonary artery to the recipient’s, and the aorta to the recipients.
Step 4: Reperfusion and Weaning from Bypass
Removal of aortic cross-clamp allows blood flow into donor heart, warms and restores contractions.
The bypass machine slowly removed as heart resumes pumping again and then monitor hemodynamic stability. The sternum is wired together, and chest incision closed with sutures or staples.
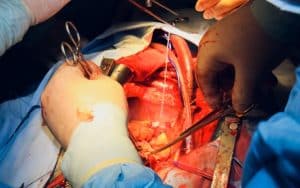
Fig. Heart transplantation
Immediate hyperacute rejection possible up to 1-week post-allograft despite immunosuppression post-revascularization.
Transplant patients need infection prevention to avoid bacterial infections during post-transplant period.
Steroid therapy after transplant surgery can cause psychiatric issues, which can be prevented with evaluation.
Allograft vascular disease leads to late graft failure and death, with concentric myointimal hyperplasia in coronary arteries as early as 3 months.
Long-Term Complications as follows:
Chronic Rejection and Cardiac Allograft Vasculopathy
Chronic Kidney Disease
Diabetes Mellitus
Malignancies
Hypertension
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



