
Blood transfusions date back to early civilizations, even the ancient ones, but it was already in the 17th century when a milestone of blood circulatory and compatibility research was reached. In fact, the work of William Harvey on the circulatory system of 1665 laid the groundwork for the blood transfusion interventions we see today in practice. In the early 19th century, the blood transfusion history was quite unsuccessful due to the lack of knowledge about blood compatibility, which caused severe reactions like hemolysis. These were met with the discovery of Karl Landsteiner in the year 1901. He discovered a blood group system named ABO and came up with the safest way to conduct blood transfusion. Standard blood typing and mixing tests were outlined using the accumulated knowledge which meant that the risk of the wrong blood being given to a patient was greatly reduced, and patients were getting better. Reuben Oscar Rh was the one who in 1907 discovered the Rhesus factor, thus introducing a more detailed system of blood compatibility testing. The introduction of blood banks during World War I was a breakthrough in the provision of transfusions, and it led to improved survival rates in emergency situations. At present, most blood transfusions occur as a part of treating the body and appear in everyday medical practice by being used in illnesses such as anemia, trauma, and bleeding disorders.
Blood transfusions are frequently a must for patients with specific diseases such as anemia, bleeding disorders, or even heart disease. To find out if there is a potential risk of bleeding disorders or heart disease, the patient’s medical history is to be reviewed. Even with major surgeries, blood transfusions can be inevitable because of heavy blood loss, as in the case of heart surgery and major trauma surgery. Blood typing and cross-matching are done, as well as infection if needed, to ascertain that the blood and patient matching is the same. Furthermore, detailed information about the medical doses of red cells transfused through the veins should be clearly discussed with the consent of blood. The blood transfusion is a process where the patient’s blood is infused through a vein in the arm or the hand; thus, the tried and tested method of monitoring is still the best way to guarantee the process of this treatment with the patient being free from any negative occurrences.
Blood collection bags are aseptic, which are made of PVC or polyurethane, thus they are available in different sizes to accommodate various blood volumes. Blood collection sets are made up of needles, tubing, and adapters which are used to connect the donor’s arm to the blood collection bag, thus air bubbles are minimized, and blood flow is smooth. On the one hand, needle holders serve as needle confinement devices during the collection process, and on the other hand, arm boards are used in order to comfort and support for easy needle insertion. Blood administration sets are tubes, adapts, and filters that are used to connect the blood bag to the recipient’s vein, thus air bubbles are prevented, and controlled blood administration is ensured. Blood warmers are used to warm cold blood products before administration to body temperature that helps to avoid hypothermia, which is a severe complication of blood transfusions. Infusion pumps are machines that are designed to control the speed of blood administration, whereas the pressure infuser is used in patients with rapid transfusions or low blood pressure to give blood products under pressure. Blood filters are devices that deduct small particles and material debris before blood administration, hence the chances of direct allergic reactions and undesired incidents are cut down. Intravenous catheters are inserted into a vein to provide blood access and come in various sizes and types to suit the patients’ diverse requirements.
Step-1: Before the blood transfusion: A blood transfusion is based on the details of the patient’s medical history, the current condition and the procedure performed. The patients are briefed about the hazards and advantages of blood transfusion and their signatures are obtained. Blood is typed and cross-matched to assure compatibility with the compatible donor blood. The most fundamental signs, such as blood pressure, heart rate, and temperature, are taken and stored duly.
Step-2: During the blood transfusion: A catheter is placed in a vein to gain access to a blood vessel for the transfer of blood. The blood administration set is connected to the IV line and the compatible blood bag. Blood must be heated to the body temperature level. The infusion pump controls the rate of transfusion. The vitals of a patient are constantly monitored and closely watched for allergic reactions or other complications.
Step-3: After the blood transfusion: Following a blood transfusion, the blood administration set is released from the IV line and blood bag. Vital signs are observed to make sure things are normal and stable. One of the tasks is taking care of the risk, such as the type, volume, and even the complications of such transfusions. Used equipment should be trashed in accordance with the rules for medical waste disposal.
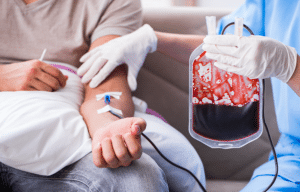
Blood transfusions can cause different reactions like fever, hives, itching, nausea, and vomiting. Specifically, fever results from the white blood cells in the donor’s blood, whereas hives are the reddened welts on the skin. The itchy skin is another very familiar one and could be the proteins in donor blood or the drugs that were given out. Hives, itchy skin, facial or throat swelling, difficulty breathing, dizziness, low blood pressure, and other indications in serious allergic reactions can even lead to death. The main symptom of hemolysis, in turn, is when the recipient’s and donor’s blood are not compatible, resulting in fever, chills, pain, dark urine, and jaundice. Circulatory overload is the condition where a large amount of blood is transfused quickly, and the symptoms can be shortness of breath, chest pain, and high blood pressure. If a transfusion-related respiratory injury is present, it may lead to a buildup of fluid in the lungs, along with dyspnea, cough, fever, and hypotension.
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



