
Arthrocentesis is the process of aspirating synovial fluid from the joint capsule for diagnostic and or therapeutic purposes. Other names are given to this process, and one of them is joint aspiration.
Arthrocentesis is utilized mainly in defining the presence and origin of joint complaints like joint pain, joint swelling, and joint inflammation. Besides, it can be used in a treatment process to reduce pain and stress on various structures within a synovial joint that contains the synovial fluid.
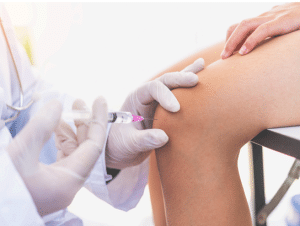
Joint aspiration
The joints within the body are surrounded by a capsule and have a small volume of synovial fluid. This fluid acts as a base on which the joint surface comes into contact rubbing against each other and feeds the joint. Changes to the regularity of specific components of this fluid can therefore be employed as a basis for deriving various details concerning the pathology of joints.
Sterile gloves
Sterile drapes and towels
Sterile dressing materials (e.g., adhesive bandages)
A sterile container for collected synovial fluid
Sterile syringes (10-20 ml) and needles (usually 18-22 gauge)
Sterile collection tubes for synovial fluid
Antiseptic solution for skin preparation
Local anesthetic
Laboratory requisition form
Waste disposal container for sharps
Patient Assessment: It is necessary to obtain a thorough medication history including allergy history, coagulopathies, current medications, past medical and surgical or any prior musculoskeletal history.
Evaluate the patient’s health status and measure their general physical status, such as blood pressure, pulse, and respiratory rate.
Informed Consent of patient: Get a consent from the patient so they will have adequate knowledge of what is being done to them.
Local anesthesia: To lessen discomfort during needle insertion, numb the region surrounding the joint using a local anesthetic.
When doing the arthrocentesis, wait for the anesthesia to wear off.
Synovial Fluid Collection: Provide enough synovial fluid to enable tests to be done or to receive enough for diagnosis, which could be in milliliters.
When the sample has been collected, label it properly, along with the patient data and the name of the joint.
Observation: Observe any changes in the patient’s vital signs and the joint throughout the procedure to see if there are any complications like infection or bleeding.
Post-Procedure Care: Cover the site where the needle was inserted with a clean or sterile dressing pad/ plaster.
Supervise the patient for early postoperative adverse effects arising due to the procedure.
Patient Position:
Get the patient in an appropriate position, to enable you have easy and correct angle to insert the needle into the targeted joint.
Arthrocentesis or joint aspiration is the puncture process, the procedure of drawing off synovial fluid from a joint cavity for diagnostic or therapeutic purposes. This method can be slightly varied depending on the joint considered to be aspirated and the patient’s status.
Knee Joint Aspiration: The patient should be in a supine or sitting position of the hip in at least 90 degrees of extension or slightly flexion.
Distract the skin gently to identify the patella and prepare to pass the needle slightly inferior on the medial or lateral side of the patellar tendon, just below the patella’s lower edge.
Hip Joint Aspiration: The affected hip should face up when the patient lies in a lateral recumbent position.
Place the needle, so that it contacts the skin close to the femoral neck and the greater trochanter, and direct towards the centre of the hip. It should be implanted posteriorly and slightly inferior to the profile of the greater trochanter.
Shoulder Joint Aspiration: It is recommended that the patient should either sit or be positioned, depending on the operator’s preference.
Introduce the needle beneath the acromion usually slightly outside the coracoid process to reach the glenohumeral joint. The direction in which the needle should be placed should be slightly posterior and inferior.
Elbow Joint Aspiration: The position that the patient should be seated in is with a 90 degree at the elbow and the forearm should be pronated.
Make the injection in the soft area below the olecranon process toward the olecranon fossa of the elbow joint.
Wrist Joint Aspiration: Identify the radial and ulnar styloid process, which are seen as two projections located at the wrist.
Make the puncture just proximal to the styloid processes of the radius and ulna, in the direction towards the radiocarpal joint between the radius and the carpal bones.
Ankle Joint Aspiration: This should be done with the patient seated or in a comfortable position with any movement immobilised at the ankle joint.
Make the injection just above the lateral malleolus or the medial malleolus according to operator’s convenience targeting the tibiotalar joint in the ankle.
Pain and Discomfort: There may be a little discomfort at the time of the procedure, most of which is felt when the needle is being inserted. This can frequently be treated with local anesthetic agents.
Bleeding: Hemorrhage at the site where the needle was inserted is another complication that can be observed in patients. More often, this is of a minor degree and transient but in patients who have bleeding disorders or patients those taking anticoagulant agent, it can be more significant.
Infection: There is a chance of infecting the joint even using sterile methods.
This can lead to septic arthritis a severe complication that, requires an urgent attention.
Joint Damage: Conduction of the procedure poses a threat of straining joint structures like ligaments, tendons, or cartilage, mainly when conducted by an inexperienced operator.
Joint Instability: In some cases, the procedure may result in some form of instability of the joints, mainly in patients with joint problems.
Post-Aspiration Pain and Swelling: The patient may experience pain and joint swelling after the procedure; this is, however, normal.
LEARNING & CME
View All
Advanced
Cardiovascular
Life Support

Basic Life
Support

Pediatric
Advanced Life
Support

Neonatal
Resuscitation
Program

Annual Stroke
Center
Continuing
Education

Opioid and Pain
Management

National
Institutes of
Health Stroke
Scale

Basics of
Electrocardiography



